
Proper Use of Tourniquets
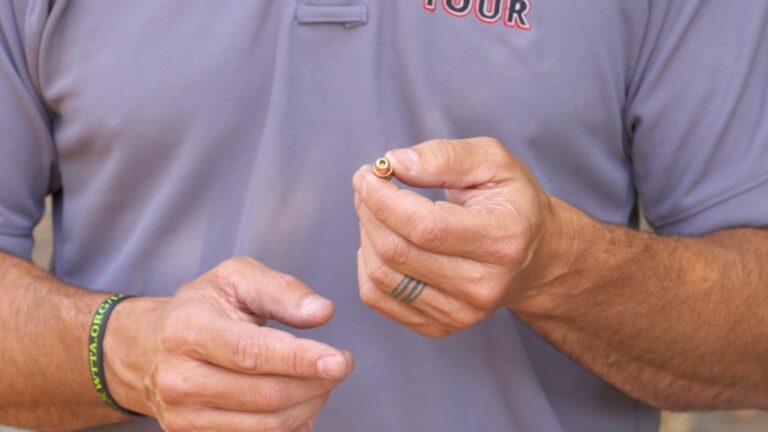
Rob PincusRob Pincus demonstrates the proper use of a tourniquet to treat an injury. A Personal Defense Network (PDN) original video.
Share tips, start a discussion or ask one of our experts or other students a question.
Make a comment:
Already a member? Sign in
4 Responses to “Proper Use of Tourniquets”
Explore videos by Rob Pincus
You may be interested in
Premium Membership
Unlock exclusive member content from our industry experts.
- 24/7 Access to Premium Personal Defense and Firearm Training Videos and Drills
- Step-by-Step Instructional Demos and Guides
- 50% Off Video Downloads Purchased in the Personal Defense Network Shop
- Access to Ask the Expert Program
Unlock exclusive member content from our industry experts.
- 24/7 Access to Premium Personal Defense and Firearm Training Videos and Drills
- Step-by-Step Instructional Demos and Guides
- 2 Full-Length Video Downloads to Watch Offline
- 50% Off Video Downloads Purchased in the Personal Defense Network Shop
- Access to Ask the Expert Program
Gold Membership
$340 Value
Get everything included in Premium plus exclusive Gold Membership benefits.
- 24/7 Access to Premium Personal Defense and Firearm Training Videos and Drills
- Step-by-Step Instructional Demos and Guides
- 9 Full-Length Video Downloads to Watch Offline
- 2 Full-Length Personal Defense Classes to Keep for Life
- 2 In-Depth Skill Development Presentations
- Discounts on Purchase-to-Own Content in the Personal Defense Network Shop
- Access to Ask the Expert Program
- Exclusive GOLD LIVE Streaming Events
Get exclusive premium content! Sign up for a membership now!








































































Lone Star Medic: I don't doubt that tourniquets can be safe, if applied by trained medics using proper procedures. But many viewers of this video do not have medical training, or access to those particular products that you mention. When most people think tourniquet, they envision something like a rope or article of clothing, tied with a knot, and a stick or tool inserted to provide torque when twisting. And you seem to miss my last sentence, which gave an exception for life threatening bleedouts. When creating an instructive video like this one, you have to consider the audience and how they will interpret the information. In this case, there are likely many people who will not understand the finer points and procedures that you have in your mind as basic assumptions.
Anatomically and physiologically speaking; the brain must continue to function in order for the rest of the body to. The body may continue to function without the use of all the other organs, such as the spleen or even other body parts of the body like an arm or a leg. But if the brain stops, everything else stops; immediately. So we need to keep the brain working by feeding it. We feed it by giving it several things such as sugar and oxygen for example. Well if there is no blood left to send that sugar or oxygen to the brain, the body dies; immediately. This is bad. Another reason we no longer use the acronym “ABC” when assessing a patient. Instead we use “CAB” so as to identify and treat moderate to severe external bleeding first (the Circulation part); then assess a patient’s Airway then Breathing… in that particular order. If this still doesn’t make sense, I encourage you to attend a training course that teaches such modern-day techniques and why we do utilize tourniquets as such.
I guess the Committee on Tactical Combat Casualty Care (CoTCCC), over 12 years of combat on two fronts with thousands of injuries and deaths, and a simple understanding of human anatomy and physiology accounts for nothing, Denver? Regarding your reasons you think this is bad advice: 1. Yes if the tourniquet (tq) is applied too tight it can tear tissue instead of occluding blood flow. This happens more often with certain tq's than other brands. I have not been able to find any documented cases of either the CAT or SOFT T Wide causing such an injury. To do so would require a great amount of force and more than likely either one of these two tourniquets would break apart before that could happen. If you are worried about "losing the limb"; please show me any documented case in the history of tq use in a pre-hospital setting where the patient lost a limb due to an extended time frame. Also, let us not forget that if we don't stop the bleeding, then we lose the entire patient. So do we want to lose or do we want to lose big? “Well doctor, we saved the limb… but the patient bled out and died. But hey! We saved the limb.” 2. There are several recent (past 15 years or so) well documented case studies that prove that a tq can remain tight and left on a limb for up to six to eight hours before the concern of necrotic tissue. Granted it is a topic of discussion right now with CoTCC and other healthcare professionals on what pre-hospital protocols should be considered after that initial six to eight hours. Yes, there is a risk of circulating necrotic cells and the toxins related to necrotic tissue/cells throughout the human body resulting from either a penetrating traumatic injury or from tq use past the 6-8hr mark. Not to mention the fact we also risk circulating clots throughout the body. Which can cause pulmonary embolisms and that is bad for the patient. In regards to the old school of thought by "elevating the limb" first; this has proven to be absolutely useless and a complete waste of time on the battlefield. Now we may not be on a battlefield here back home, but bleeding is bleeding. When dealing with moderate to severe bleeding, time and blood are two things we don't have a lot of. The average human adult only has about five to six litters of blood in their body. Once blood has been spilt on the ground, we can’t put it back in the body. Therefore we need to save and maximize as much as we possibly can... as effectively and efficiently as we can.
This video gives bad advice. There is good reason a tourniquet in an option of last resort for stopping bleeding. 1. If it is applied too tight or for too long, the tissue in the extremity can die and you will lose your arm or leg. 2. With the tourniquet applied, blood remaining in the extremity will begin to degrade because of lack of circulation. In this case when the tourniquet is removed the toxins in the blood will flood your circulatory system and can cause septic shock and lead to death. Always try direct pressure and elevating the limb first. There is no reason to risk using a tourniquet unless there is a life threatening bleedout occurring.